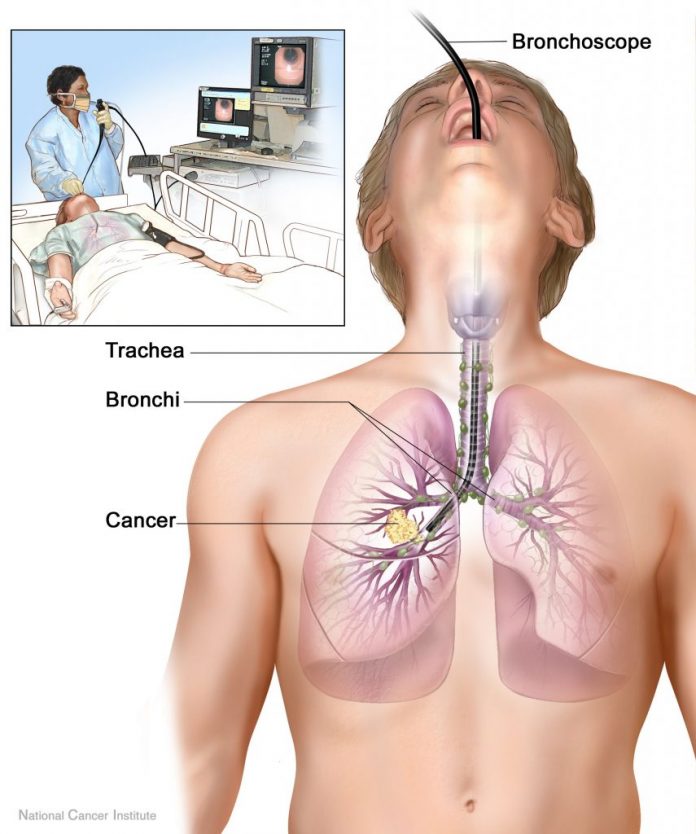
The Bronchoscopy
Like the tree has a stem which divide multiple times in to branches to form twigs, our respiratory system has the main airway, the trachea, which further divides multiple times (bronchi) to form very small air pipes- the bronchioles. Like the leaves breathe for the tree, the alveoli breathe for us. Yet, something can go wrong in this harmonious natural system and we- the doctors, try to search for an answer for cure.
Fibre-optic bronchoscope is the device usually used by pulmonologists to look into the wilderness of our lungs. It is about as thin as a pencil, flexible with camera and fibre-optics allowing light to shine at the tip. There is also a hollow channel within that allows collecting specimen and passing various instruments.
Who requires a Bronchoscopy?
Mainly it is used for diagnosis of conditions which are persistent and unusual. For example, persistent cough, cough with blood or strange shadows on a chest x-ray. A tissue sample thus taken is visualized under the microscope to help decide whether the problem is inflammation, infection or cancer.
It can also be used to treat certain conditions. With the help of different kinds of instruments we can remove foreign objects (inhaled peanut), put a small tube (stent) to open a closed airway due to cancerous growth within or remove thick secretions blocking the airway.
How is it done?
The procedure is usually a day case or outpatient. It is done under local anesthesia which numbs the inside of the nose and throat and under sedation which can make you drowsy but does not put you to complete sleep as in general anesthesia. However, in most of the situations, you are not likely to remember anything of the procedure. Heart rate and blood pressure is regularly monitored throughout the procedure. Depending on case to case basis the side effects vary and the procedure can last from 15 to 45 minutes.
Recently we conducted two successful bronchoscopies at Bahrain specialist hospital. Our first patient was a young 19 year old boy who presented to the hospital with ARDS (acute respiratory distress syndrome) a life threatening condition. After stabilizing the patient bronchoscopy was conducted and a fungal species called Penicilliumwas identified. Our second patient was an elderly gentleman of 74 years having multiple serious co-morbidities with recurrent fever and difficulty in collecting sputum for analysis. It excluded endobronchial neoplasia. Both the patients have been successfully treated and had smooth course of management.